
The lingering effects of the pandemic on what was once our “normal” lives have been difficult to overcome for many of us, especially those whose mental health was on shaky ground even before the lockdowns began two years ago. So not surprisingly, the percentage of major depressive disorder rose to 27.9% in 2020 in the adult population in the United States, more than triple the rate before the pandemic.
“We’ve learned that this statistic is most likely due to the psychological effects and long-term economic and social consequences of isolation,” says Anish Shah, M.D., a psychiatrist and founder of the Siyan Clinical Corporation in Santa Rosa. “Humans are not solitary creatures. The social restrictions, lockdowns, school and business closures and loss of livelihoods most likely contributed to this statistic. Those already living with mental health issues suffered even greater from decreased contact with other people.”
Major depressive disorder is characterized in part by a persistently depressed mood or loss of interest in activities, causing significant impairment to daily life. It can manifest with a variety of symptoms such as disturbed sleep, feelings of guilt or inadequacy, suicidal thoughts, cognitive decline, motor retardation and decreased sexual drive.
“A person has to have a certain combination of symptoms over a period of time to be diagnosed with depression,” says Kathryn Erickson-Ridout, Ph.D., a psychiatrist with Kaiser Permanente in Santa Rosa. “This includes a depressed mood or loss of interest in activities. We’ve all personally been impacted by the pandemic, which has caused so much disruption in our daily lives that many people may have symptoms of depression. But it is possible to have symptoms of depression outside of major depressive disorder. This can happen whenever there is a major stressor event, and a global pandemic certainly is one. The profound change in routine can affect people’s mood.”

Costs and risks
According to a study released last year by the Lancet Regional Health–Americas, the burden of depressive symptoms in the adult population of the United States increased over the course of the pandemic. The report states: “Mental health gaps grew between populations with different assets and stressor experiences during the COVID-19 pandemic. The odds ratio of elevated depressive symptoms for low-income relative to high-income persons increased from 2.3% in 2020 to 7.0% in 2021.”
In addition, adults between the ages of 18 and 39 had a rate of depression that increased almost three-fold during the pandemic, which was higher than any other age group, says Shah. “Younger age groups were more affected by anxiety disorders than older age groups, but seniors were still greatly affected because many were isolated from their families,” he adds. “Seniors, however, are known to have better mental health outcomes than younger counterparts,” he adds.

Since the start of the pandemic, the Lancet report stated, many studies have revealed worsening mental health across a range of populations in the U.S. and globally, including many healthcare workers, children and the general public. “Depression is costly and increases the risk for other physical and mental illness, as well as mortality,” the Lancet report concluded.
One estimate by the Centers for Disease Control and Prevention (CDC) shows that depression and anxiety cost employers $17 billion to $44 billion in 2020. In addition, as many as 200 million workdays were lost each year. “Employment benefit spending for absent employees due to COVID-19 costs employers in the U.S. approximately $50 billion, according to the Integrated Benefits Institute,” says Shah. “In California alone, it costs employers $7.2 billion.”
“The loss of 200 million workdays per year creates hidden costs that can’t easily be traced back, but we feel a substantial portion may be linked to depression and anxiety issues,” explains Khuram Arif, M.D., chief medical officer of Western Health Advantage. Based in Sacramento, this health-insurance organization has nearly 9,000 members in Sonoma, Napa and Marin counties, and 363 Behavioral Health providers in the North Bay overseeing their care.
Arif says 3% to 4% of the HMO’s 102,000 members sought out mental health services before the pandemic. Now, it’s about 40%. “That number climbed quickly in spring of 2020 and it has just sustained.”
A cry for help
In addition to the usual warning signs of depression and anxiety disorders, crying at work is another symptom, according to Arif. “Crying can be a symptom of feeling overwhelmed,” he says. “It could be the result of fear of being around people, and many are afraid to go back into offices. Isolation really changed our way of living.”
The CDC also revealed that the number of emergency department visits for attempted suicide increased by 20% in 2020 (compared to 2019 visits) with a 50% increase in girls receiving care. “Attempted suicide doesn’t necessarily mean a suicide will be completed,” says Arif. “In looking at the CDC figures on death from suicide, there was a decrease in 2020. Completed suicides didn’t climb, but attempted suicides went up sharply. Attempted suicides may be a cry for help.”

Substance abuse, or “self-treating,” also rose during the pandemic due to stress, worry and underlying psychological disorders, says Shah. “Our normal healthy coping skills such as socializing and physical activity have been limited, leaving many at home to cope with these symptoms on their own. We found that the initiation of alcohol use in individuals was 8.8% when the pandemic began, and 6.9% started smoking cigarettes. Further, 5% began using cannabis, 4.4% began using e-cigarettes, 5.6% began using stimulants and 5.6% began using opioids.”
Erickson-Ridout says Kaiser’s volume of overall psychiatric services went up by 7% [during the pandemic], particularly in substance-use disorders. “That was the largest change we’ve seen in terms of the reason the patient made the appointment and a big change from depression and anxiety to substance use and adjustment disorder. We saw substance abuse disorders increase by a little over 50% and a 53% increase in alcohol-related disorders. The problem with people turning to substance abuse to relieve their stress and anxiety is that it’s harmful to their overall health and can lead to serious medical problems. Our findings reveal that substance use disorder can also be a major player in suicide attempts.”
Safe and effective treatments
During the pandemic, the use of telehealth technology became more popular, particularly for mental health patients. “For young people especially, who tend to be more tech-savvy, they are getting a lot of their care through the virtual space,” says Arif. “Medical virtual visits with Western Health Advantage providers have been in the range of 15% to 20% of all visits conducted virtually, but our mental health visits are about 40% virtual.”
Treatment options for depression include psychotherapy and pharmaceuticals. In the past, medications for depression could have significant side effects, such as weight gain and sexual dysfunction. “But improvements have been made in these medications and these unpleasant side effects have been greatly reduced over the past few years,” says Shah.
Erickson-Ridout says antidepressant medications have good research backing them up, and by and large, are safe and effective. “They’ve been on the market for many decades, so we have good evidence supporting their efficacy and safety. Having good access to evidence-based health care works for most people, but for those who have struggled with depression without success through medications, there are other treatments available, such as transcranial magnetic stimulation (TMS). It’s a great technology that’s been around for about 30 years, and we offer it to Kaiser members.”
TMS technology has long been available for adults 18 and older but has not yet received approval from the Food and Drug Administration (FDA) to treat children. “We believe that approval is coming soon, however, probably this year,” says Shah. “TMS is also being explored for patients with PTSD and anxiety disorder, and recently the FDA approved TMS for treating obsessive-compulsive disorder.”
Coping skills suffer
A word that describes the particular kind of anxiety experienced by men, “manxiety,” has been around for several years, but the pandemic has broadened its use. Manxiety is now listed in the online Urban Dictionary and is even the subject of a podcast. More than 40 million Americans have an anxiety disorder, according to the National Alliance for Mental Illness.
How do men deal with anxiety differently than women? According to a statement released by Kaiser, men with anxiety disorders often don’t have the necessary coping skills and will turn to drugs, alcohol, gambling or destructive relationships to relieve their stress. They can become hostile and angry, and are reluctant to talk about their anxiety because they see it as a sign of weakness or a threat to their masculinity.
“Men aren’t always good at communicating health-care issues,” says Arif. “We know that men tend to seek less care overall—whether it’s medical or mental health—and women tend to be better at asking for help. A lot of jobs were lost by men during the pandemic, and there is also the stress of finding yourself in your 40s and 50s and realizing you’re not young anymore.”
Shah says he has seen depression and anxiety increase in patients who have not had COVID-19, but live in fear of getting it, or have lost a family member to the virus. “I personally have close family members and friends who were treated for the virus and recovered, and I saw a rise in depression and anxiety among them.”
“There have been a couple of studies linking a COVID-19 infection with a risk for depression and anxiety,” adds Erickson-Ridout. “In patients who recovered from having the virus, it appears they have an additional risk of having depression and anxiety as a symptom of ‘long COVID’ complications.”
Reaching out
Even with many tried-and-true treatment options available, having a good support system from friends and family can be some of the best medicine during stressful times. “A long life is linked with a strong social support system,” says Arif.
“Prioritizing time with friends, getting exercise and following a healthy diet can help protect against depression and anxiety,” adds Erickson-Ridout. “Isolation is a huge risk factor for depression, so the more people you can reach out to, the better. One of the hardest parts of coping is when your brain starts telling you that you’re alone.”
Know the Warning Signs
All of us have experienced anxiety at some point in our lives. Yet, take note: an early warning sign of anxiety and/or depression occurs when a person begins avoiding things they once enjoyed.
Warning signs for anxiety may include:
Shakiness
Increased heart rate
Tightness in the chest and/or rapid breathing
Racing thoughts
Advanced signs of a generalized anxiety disorder include:
Excessive worry occurs more days than not for at least six months
Distress or impairment in social, occupational, or other important areas of functioning
Feeling restless
Fatigue or frequently feeling tired
Difficulty concentrating
Irritability
Muscle tension
Sleep disturbances, such as difficulty falling or staying asleep
Warning signs of depression include:
Isolating oneself
Frequently thinking negative thoughts
Reoccurring feelings of sadness
Advanced signs of a major depressive disorder include:
Feeling down or depressed most of the day, nearly every day
Diminished interest in activities you once enjoyed
Significant changes in your weight (increased or decreased)
Difficulty with sleep (insomnia or hypersomnia)
Similar symptoms as noted above for generalized anxiety disorder
Recurrent thoughts of death over at least a two-week period
Source: Mayo Clinic Health System
A Noninvasive Alternative
For people with depression who have tried all other treatments without success, a noninvasive procedure called transcranial magnetic stimulation (TMS) may be the answer. TMS uses magnetic fields to stimulate nerve cells in the brain to improve symptoms of depression and is typically recommended when other treatments for depression—such as medication and psychotherapy—have been ineffective. It delivers repetitive magnetic pulses, so it’s known as repetitive TMS or rTMS.
Anish Shah, M.D., who began his practice as a psychiatrist in 2004, is the founder of the Siyan Clinical Corporation in Santa Rosa, which has been treating patients using TMS since 2016. He specializes in mood disorders such as depression, attention-deficit/hyperactivity disorder (ADHD), post-traumatic stress disorder (PTSD), substance abuse and schizophrenia.
“In the past five years our clinic has treated 207 patients using TMS,” he says. “Out of all those patients, 70% have decreased their levels of depression by 50%, and 30% of those patients reach remission. The effects of TMS are long-lasting in a majority of patients, and only about 20 of our patients have needed to repeat the TMS treatment protocol. It’s an extremely safe treatment for clinical depression, and the beauty of it is it has no side effects. Generally, when patients take medications such as antidepressants there are side effects.”
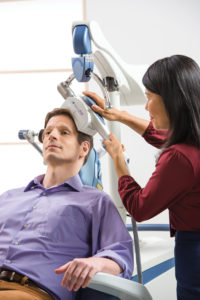
The TMS treatment protocol is a full course of 36 sessions. For five days a week for five to six weeks, patients receive a magnetic pulse to the region of the brain involved in mood control and depression. Each session lasts about 30 to 40 minutes, performed on an outpatient basis and without requiring anesthesia. At each session, an electromagnetic coil is positioned against the scalp near the forehead. The Siyan Clinical has used TMS on patients ranging in age from 18 to 80. Shah says most private health insurance and Medicare covers the cost of TMS treatments.
Is TMS therapy right for you?
According to the clinic, TMS therapy may be right for you if you agree with one or more of the following statements:
- Depression symptoms have interfered with my daily life.
- I am not satisfied with the results I get from depression medication.
- I have had or worried about side effects from depression medication.
- I have switched medications for depression due to side effects.
- I am interested in an FDA-approved and scientifically-proven, non-drug therapy for depression.
Teens and Suicide
A study by Kaiser Permanente found there was a small uptick in suicide-related emergency department visits among teen girls in the fall of 2020. Authored by Kaiser psychiatrist Kathryn Erickson-Ridout, M.D., Ph.D., the study revealed that the number of teens being seen for suicidal thoughts and behaviors in Kaiser emergency rooms in Northern California did not increase significantly during the pandemic, though specific groups of teens may have sought care at high rates during late 2020.
The findings, reported in JAMA Psychiatry in September, showed an overall reduction in the number of suicide-related emergency department visits by patients ages 5 to 17 between 2019 and 2020, decreasing from 2,339 to 2,123. Approximately two-thirds of the visits were by girls ages 13 to 17. Suicide-related visits are those coded for suicide attempts, suicidal ideation and self-injurious behaviors.
“There is widespread concern that there has been a big increase in mental health crises among teenagers because of the pandemic,” says Erickson-Ridout. “But these findings suggest that the trends over time are generally consistent with the year prior to the pandemic, though there may be certain individuals who need more attention.”
Suicide is the second leading cause of death among teenagers in the United States.
Author
-

Jean Doppenberg is a lifelong journalist and the author of three guidebooks to Wine Country.
View all posts



