
There’s a new kind of killer on the loose in the North Bay. It lurks in disguise, waiting for kids looking for a good time, or older people just looking for a little relief beyond what the docs prescribe. It’s colorless, tasteless and just the tiniest amount can kill. And it fits right into a familiar-looking little pill. It’s fentanyl. And the number of lives it takes just keeps climbing–– one death a week, more than two non-fatal overdoses a day, in Marin, in December of 2020. “Our experience in Marin is shared with most of the nation,” says Marin County Public Health Officer Matt Willis, MD. “The waves that you can see happening across the nation are visible in Marin and across the Bay Area.”
He describes the opioid crisis as having come in three waves. The first wave, starting around 1995, was driven by a flood of advertising—backed by misleading assurances from the pharmaceutical industry—prompting well-meaning physicians to begin liberally prescribing this supposedly miracle, non-addictive drug. The miracle drug, Oxycontin, tragically turned out not to be as advertised—and numbers of people in chronic pain were becoming addicted and worse. The Centers for Disease Control reports that across the nation, from 1999 to 2020, more than 564,000 people died from overdose involving opioids. “Primary care clinicians like myself were in fact over-prescribing painkillers,” says Dr. Willis. “Because we were being given bad information.”
Willis had his awakening moment in phase one of the crisis. “I had been working as a primary care doctor in Marin County for a year before I became public health officer and I recognized that many patients I had inherited, from someone who had retired, were taking what I thought to be high doses of opioids, sometimes in combinations with other medicines that I knew could be dangerous. And it was seen as normal among my fellow practitioners.”
At the same time, he says, “When I became public health officer looking at the data, we saw this alarming trend that the leading cause of accidental death in the county was in fact opioid overdose. And most of those overdoses were due to prescription painkillers.”
The Coalition
The second phase, around 2013, came as new regulations began to clamp down on prescriptions, and opioids became less readily available—driving an increase in heroin use, along with death by overdose. In 2014, Dr. Willis met with Marin parents who had seen too many kids die and were concerned that not enough was being done to curb the opioid crisis. Among them were Mark Dale, who almost lost his son, and Susan Kim, who lost her son to a prescription drug overdose. Together, with the support of Marin Health and Human Services, they formed RX Safe Marin, the Opioid Safety Coalition, to address the crisis of prescription drug misuse.
“We formed a coalition to recognize that opioid use is a complex problem that touches people across Marin and every community, and actually relates to every sector,” says Willis. “So, we needed new infrastructure, a process for engaging in conversations across healthcare providers, law enforcement, schools, pharmacies and substance-use service providers.” They needed to create a shared understanding of the nature of the problem so they could come up with shared strategies. The coalition model was the only reasonable approach, Willis explains, “because it sits above and outside of any one of the sectors who come to the table.
“It convenes a kind of conversation that can only happen when you get everyone together.”
To make any significant impact, everyone needed to acknowledge and understand the common problem and come to the table together. “So,” he laughs, “you literally had people with, you know, guns and badges sitting next to people with stethoscopes.” The coalition would then become its own entity, with a presence greater than the sum of the individual sectors. “And the best solutions are somewhere in between all those agencies,” he says.
RX Safe Marin becomes OD Free Marin
But a new wave in the crisis was forming. By 2018 prescription drugs were more under control and then heroin receded—just as a synthetic opioid called fentanyl came on the scene. It’s 100 times more powerful than morphine, 50 times more powerful than heroin, able to blend into almost anything—and lethal at just a few grains. Fentanyl is the killer now. Since 2018, the overdose death rate has continued to rise.

Then, he says, “following the data on overdoses, we started seeing a different pattern.”
What they were seeing was a rising number, in Marin and elsewhere, of overdoses not from prescription drugs, but from illicit substances. “At that point fentanyl was just emerging,” he says. “We were seeing heroin, methamphetamine, cocaine, just a wider range, as well as prescription medications.” But the problem of over-prescription of opioid medications had really diminished. “And yet our action teams, and in fact our name, was really still oriented toward that first, prescription opioid wave of the crisis.” They started talking about adjusting their strategic design in 2020 when COVID hit and put a pause on recalibrating the program.
As the immediate dangers of COVID subsided throughout 2022, RX Safe Marin began looking again on how to adjust its focus to the new wave of the opioid crisis: overdosing and death not by prescription drugs but by illicit substances—packaged like prescription drugs but bought outside the legal system. These overdoses were becoming epidemic. In October 2022, the coalition changed its name to OD Free Marin.
“With OD Free Marin,” says Willis, “we are more formally dedicated to the problem of overdose and drug poisoning. That’s where all of these issues converge. In this new phase, the coalition approach has proven even more important.” It takes all sectors to understand, to communicate, to see the same information and to work together to save lives, adds Willis.
“We’re fortunate to have partners who want to come together,” says Willis. “I think that’s another asset for us in Marin, that, by and large, it is a community-minded group. Ultimately, everyone wants the same thing. And so the conversations very quickly get to the ‘how,’ more than the ‘whether.’”
Adds Willis: “Our strategies now focus on education and awareness, access to treatment, and to Naloxone, the anti-overdose medicine.”
The coalition wants to avoid concepts of blame, or shame or arresting people. It’s about making sure everyone in the community knows that unwitting young people are dying in shocking numbers, and that there are ways to keep them safe. OD Free Marin wants to educate about how to keep safe, if they’re users, or to make sure their kids keep safe, if they’re parents of users.
First, take away the stigma
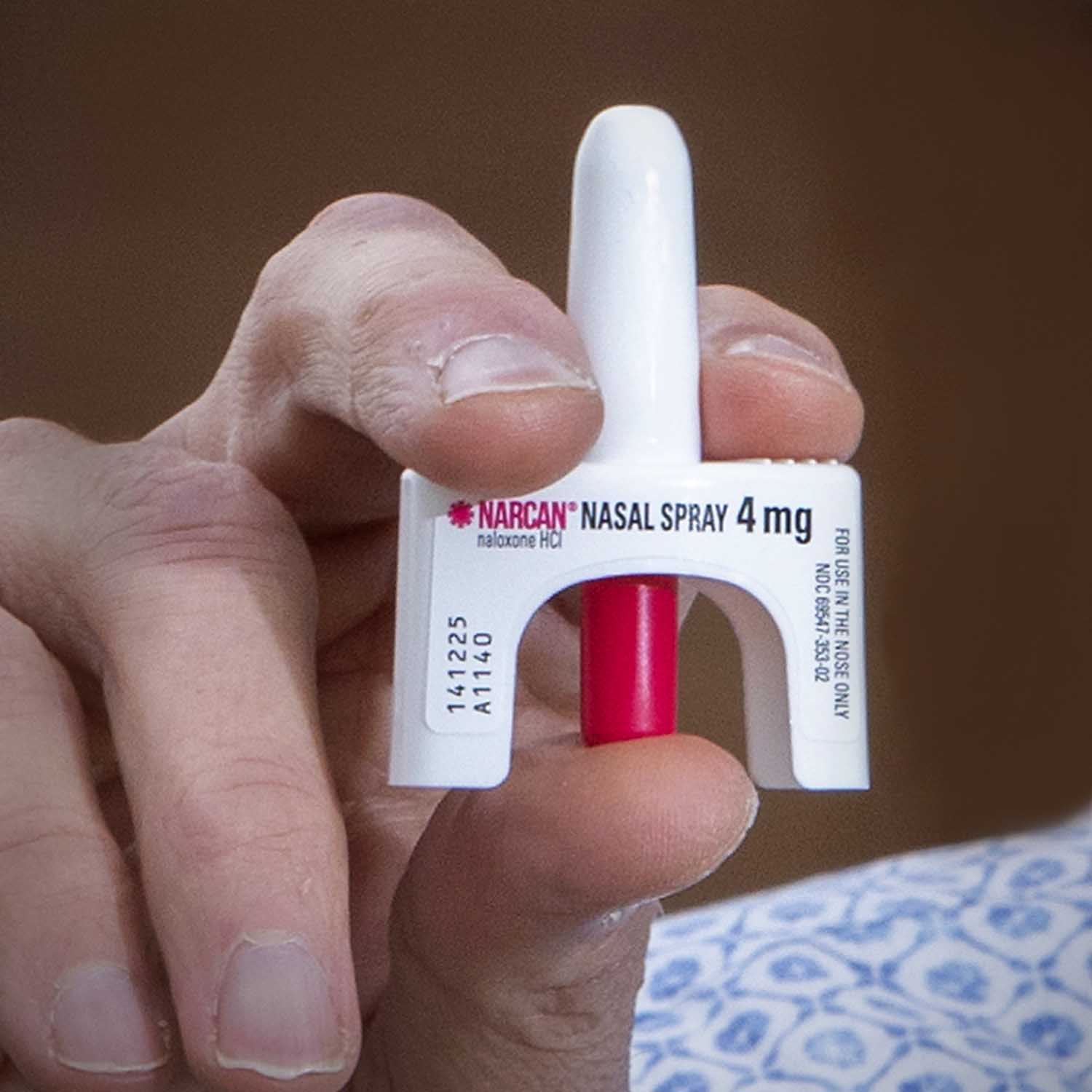
“Most of our fatal overdoses are due to people who’ve taken pills,” says Dr. Willis. “More so than ever because fentanyl often finds its way into pill form.” Fentanyl, as a powder, can be easily added to almost any other substance. And more than half of the counterfeit pills now seized by the DEA contain fentanyl. Thus, experimenting with pills from a non-regulated, illegal source is like playing Russian Roulette.
The antidote, Naloxonen, or Narcan, is kind of a miracle drug. It is a nasal spray and has virtually no other downsides or side effects, aside from reversing the effects of an opioid overdose. It binds to the receptors in the central nervous system to which the opioid binds. When someone has an experience of being high from an opioid, the person feels euphoria, but they also lack the automatic impulse to breathe. And so when someone overdoses, they lose consciousness and can stop breathing. When one is under the influence of opioids, that drive to breathe is turned off—often resulting in accidental death.
A Mother’s story

Greenbrae resident Michelle Leopold understands this. She lost her 18-year-old son to a counterfeit pill in November 2019 and has now become an activist and organizer, educating parents, young adults and communities about how to save young people from fatal accidental opioid overdose, or “fentanyl poisoning,” as she calls it.
“It was three years ago that Trevor died,” she says, “and there were two other Marin boys that I knew of that died just a couple of months after, also from illicit fentanyl.” In the days after his death, she decided to turn her grief into practical use and to speak out. “So, Trevor died at Sonoma State [University],” she continues. “He had bought pills and he and some friends had used some of the pills on Friday night. And then he took one of the pills, or I think it was the last one, on Saturday.” He took the pill, went to sleep and did not wake up. Why? The pills, bought from an unregulated source, as many are, were marked “Blue 30s,” meaning Oxycodone. He thought he was using Oxycodone, not fentanyl. But the toxicology report showed no Oxycodone in the pill. “It was a fake pill,” says Michelle. “I believe that if fentanyl wasn’t in the mix, Trevor would still be alive.”

Without that one deadly pill, Trevor might still be struggling—as he had been struggling with addiction—but he’d be alive, his mother insists. “And that’s one of my arguments when people say, you know, that he died from an overdose. I’d say: No. He was intending to take Oxycodone. He was not planning on taking fentanyl. He had a friend over, in his dorm room that night. He did not intend to die.”
She wants parents to understand: this current drug scene is different from what they may have experienced in their generation. Innocent looking pills may not be what they claim to be and can kill your child. Even today’s legal marijuana can contain high levels of THC and can make a person violent, not mellow, as Michelle experienced with Trevor’s diagnosed Cannabis Use Disorder. Michelle also talks about today’s high-potency marijuana products, explaining that parents and their children need to know are different from what people were used to in previous generations. This makes her angry. So, she speaks out. “I especially want to educate young adults primarily,” she says. “To tell them, do not take any pills unless you personally were prescribed them and you personally picked them up from the pharmacy. If you get it from a pharmacy, and you pick it up at a pharmacy in the United States, then it is safe.” But if you get it from your friends, from your friend’s supplier, or from the Internet, beware: It may be cheaper, but you could pay with your life.
She also talks about Narcan, the antidote. “Narcan has a place, and it will save lives,” she says. “If Trevor’s friend had known what to look for in signs of an overdose, and if she had had Narcan, Trevor would most likely be alive right now.”
Hear it from a student
Novato High School student Jessica Mendieta, 16, has been working in social justice for three years. Now, as a member of OD Free Marin’s Youth Action Team, she is an active proponent of Narcan training and availability. She says getting the word out is urgent. Getting the right word, the right message, is even more urgent.
It’s no longer the old “just say no,” which for the vast majority of young people simply didn’t work. Now, when the stakes are about life and death, the message Mendieta wants to get across is about how to use—if you must—but stay safe; how to experiment with drugs as some young people do––and stay alive. This is a new approach to a new reality.
 Do students talk to students about this? “It varies,” says Mendieta. “My friends and I, we’ve talked about it, but I know there are other people who are kind of living in––I wouldn’t say ignorance, but they’re just not as aware, they don’t really understand the gravity of it. Like, there’s a high chance that it could be you next!” Any user—even those just going along with everyone else—could suddenly, accidentally die, she stresses. It is happening, and the point she wants to get across is: Know how to keep yourself safe. “Because,” she says, “it’s just so prevalent.”
Do students talk to students about this? “It varies,” says Mendieta. “My friends and I, we’ve talked about it, but I know there are other people who are kind of living in––I wouldn’t say ignorance, but they’re just not as aware, they don’t really understand the gravity of it. Like, there’s a high chance that it could be you next!” Any user—even those just going along with everyone else—could suddenly, accidentally die, she stresses. It is happening, and the point she wants to get across is: Know how to keep yourself safe. “Because,” she says, “it’s just so prevalent.”
To the parents of friends who may be experimenting with various substances on a recreational basis, her message is unambiguous: Many teenagers experiment with drugs. They just do. And, whether parents believe it or not, their kid might be using some drugs at one point or another, even if only to experiment. But the death pill is out there. So they should know how to be safe. They should never use alone, and always have someone who can administer Narcan, the “anti-overdose” medicine that now, thanks to the work of OD Free Marin, is readily available just about everywhere. Included in her message is that those using drugs should know how to use test strips to make sure there’s no fentanyl in whatever they’re using. The strips aren’t perfect––the test can miss other, almost-equally lethal substances. To be truly safe, people using drugs should have someone with them so that, if they pass out in an overdose, “someone’s there to call for help.”
“But really,” she says, “it’s just about having an honest conversation with your kid to explain to them the gravity of the situation that if they’re going to use, they should take extra care when they do.”
Mendieta and the OD Free Marin coalition work to help the community recognize that Narcan should be without stigma and on hand wherever drug use may take place: in schools, at homes, around the community. It’s easy to apply and has no side effects, other than potentially saving a life. Someone can spray Narcan up the unconscious person’s nose and almost immediately, as long as blood is still flowing, the Narcan will restore the normal functioning of the central nervous system and the unconscious person will begin to breathe. “It’s super effective at reversing an overdose,” says Dr. Willis, but adds “Narcan is not the ultimate solution. One of the strongest risk factors for a fatal overdose is a history of a non-fatal overdose,” he says.
This is a complex problem and that’s why Marin County engages a holistic and integrated approach that can best be achieved through a community-wide coalition that brings together all sectors that touch the issue.
Reality is not nice to look at–but it’s there anyway
“It’s remarkable to me,” says Willis, “even at this stage with more than one death a week, more than two overdoses per day, that our young people are still purchasing counterfeit pills on the Internet and dying. It’s obviously a failure of understanding.” And the crisis is accelerating. With 2022 another record year, his goal for 2023 may seem modest: “Our goal is to have fewer overdose deaths in 2023 than we had in 2022.” Why not a goal of zero? “Our long term vision is to eliminate preventable deaths. But it’s a complex problem, and we know the factors that are contributing to this trend are strong and will continue, so we need to set a realistic goal for our work together this year.” OD Free Marin needs all hands to the pump to save lives.
Micah’s Hugs
Another family working to raise awareness about the deadly dangers of opioid addiction is that of Micah Hamlow-Sawyer, Jr., a Sonoma County resident who died of a fentanyl overdose in 2019 at the age of 22. Out of grief and a determination to prevent further loss of life, his father and stepmom, Micah and Michelle Sawyer, established Micah’s Hugs, a nonprofit dedicated to educating youth of the dangers of substance abuse and fentanyl poisoning—and to break the stigma that follows the disease of addiction.
 Among its services, Micah’s Hugs—named for Micah Jr.’s “bear hug” embracing of family and friends—trains community members in the use of Narcan nasal spray, which can reverse the deadly effects of a fentanyl overdose.
Among its services, Micah’s Hugs—named for Micah Jr.’s “bear hug” embracing of family and friends—trains community members in the use of Narcan nasal spray, which can reverse the deadly effects of a fentanyl overdose.
“We think everyone should be Narcan trained,” Michelle says, adding that recent trainings have included delivery personnel, truck drivers and others whose work finds them criss-crossing communities on a daily basis.
The organization also allocates fentanyl-testing strips throughout the community. And, as part of its efforts toward addiction recovery, the nonprofit provides scholarships for six-week programs at Pura Vida recovery center in Santa Rosa. In the last two years, Micah’s Hugs has provided 36 scholarships, says Michelle.
For information on scholarships or to arrange a Narcan training, visit Micahshugs.org.
How can you recognize and reverse a fentanyl overdose?
What are the signs of fentanyl overdose? Fentanyl kills by deactivating the automatic impulse to breathe. Signs are: constricted pupils; asleep, unconscious; slow or no breathing; choking or gurgling; limpness; clammy skin, discolored lips and nails.
What to do for someone who has overdosed?
- Call 911
- Administer naloxone (Narcan) if possible, which can reverse the effects of fentanyl immediately;
- Try to keep the person awake and breathing;
- Lay the person on their side to prevent choking;
- Remain with the person until help arrives.
Oxycodone: what it is, what it can do, how to be safe
Oxycodone is an opioid pain medication available legally and safely by prescription, or illegally without a prescription. The drug can become addictive and taken to excess or, in a means designed for a quick high, can lead to overdose. An overdose can cause brain damage or death. The remedy in case of overdose is Naloxone. For information about the effects of oxycodone, and how it may be combined with other drugs, such as Percocet, Oxycocet and Endocet, visit camh.ca/en/health-info/guides-and-publications/straight-talk-oxycodone.




41 thoughts on “A Death a Week: Marin Confronts its Growing Fentanyl Crisis”
Excellent work and article from Parents, Marin County, Dr. Matt Willis.
Excellent read, I just passed this onto a colleague who was doing some research on that. And he actually bought me lunch as I found it for him smile Thus let me rephrase that: Thanks for lunch!
Undeniably believe that which you said. Your favorite reason appeared to be on the internet the easiest thing to be aware of. I say to you, I definitely get annoyed while people think about worries that they just don’t know about. You managed to hit the nail upon the top and also defined out the whole thing without having side effect , people could take a signal. Will probably be back to get more. Thanks
WONDERFUL Post.thanks for share..more wait .. …
Together with the whole thing which seems to be developing within this subject matter, all your points of view are quite stimulating. On the other hand, I beg your pardon, but I can not give credence to your entire plan, all be it refreshing none the less. It looks to everybody that your opinions are not entirely validated and in actuality you are generally your self not really wholly convinced of the argument. In any event I did appreciate examining it.
Hello there! This post could not be written any better! Reading this post reminds me of my good old room mate! He always kept chatting about this. I will forward this page to him. Fairly certain he will have a good read. Many thanks for sharing!
Hello.This post was really motivating, particularly since I was looking for thoughts on this matter last Friday.
Thanks for the sensible critique. Me & my neighbor were just preparing to do some research about this. We got a grab a book from our local library but I think I learned more from this post. I am very glad to see such fantastic information being shared freely out there.
Undeniably believe that that you said. Your favorite reason appeared to be on the web the simplest thing to bear in mind of. I say to you, I certainly get annoyed whilst other people think about issues that they just don’t realize about. You controlled to hit the nail upon the top and defined out the entire thing without having side effect , other folks can take a signal. Will probably be again to get more. Thanks
Hello, you used to write fantastic, but the last several posts have been kinda boring?K I miss your great writings. Past few posts are just a little out of track! come on!
I’d have to examine with you here. Which is not one thing I usually do! I take pleasure in reading a post that may make folks think. Additionally, thanks for permitting me to comment!
I liked as much as you’ll receive performed right here. The sketch is tasteful, your authored subject matter stylish. however, you command get bought an edginess over that you wish be delivering the following. ill no doubt come more previously once more since exactly the same just about a lot regularly within case you shield this increase.
Some genuinely fantastic information, Gladiolus I detected this.
I adore gathering useful info, this post has got me even more info! .
Today, I went to the beachfront with my children. I found a sea shell and gave it to my 4 year old daughter and said "You can hear the ocean if you put this to your ear." She put the shell to her ear and screamed. There was a hermit crab inside and it pinched her ear. She never wants to go back! LoL I know this is entirely off topic but I had to tell someone!
Today, considering the fast way of living that everyone is having, credit cards have a big demand throughout the market. Persons coming from every area of life are using the credit card and people who are not using the card have made up their minds to apply for even one. Thanks for giving your ideas on credit cards.
It’s my belief that mesothelioma is definitely the most deadly cancer. It has unusual traits. The more I really look at it a lot more I am certain it does not work like a true solid human cancer. In the event mesothelioma can be a rogue viral infection, therefore there is the potential for developing a vaccine as well as offering vaccination to asbestos subjected people who are open to high risk of developing long term asbestos related malignancies. Thanks for discussing your ideas about this important health issue.
Nice read, I just passed this onto a friend who was doing some research on that. And he actually bought me lunch as I found it for him smile Thus let me rephrase that: Thank you for lunch! "Remember It is 10 times harder to command the ear than to catch the eye." by Duncan Maxwell Anderson.
fantastic points altogether, you simply won a new reader. What might you recommend in regards to your put up that you simply made a few days in the past? Any certain?
Thank you for any other great post. The place else may just anyone get that type of info in such an ideal method of writing? I’ve a presentation subsequent week, and I am on the look for such information.
Thanks for another fantastic post. Where else could anybody get that kind of info in such an ideal way of writing? I’ve a presentation next week, and I’m on the look for such information.
It is actually a nice and helpful piece of information. I am glad that you simply shared this useful info with us. Please stay us up to date like this. Thanks for sharing.
It¦s really a cool and helpful piece of info. I am glad that you just shared this helpful information with us. Please keep us informed like this. Thank you for sharing.
I am now not certain where you’re getting your information, but good topic. I needs to spend a while learning much more or working out more. Thanks for great information I was searching for this information for my mission.
Your place is valueble for me. Thanks!…
I will right away take hold of your rss as I can’t in finding your email subscription link or e-newsletter service. Do you have any? Kindly permit me understand so that I may subscribe. Thanks.
It¦s really a nice and useful piece of info. I am satisfied that you simply shared this helpful info with us. Please stay us up to date like this. Thanks for sharing.
Deference to op, some great selective information.
Dead pent content, Really enjoyed examining.
It¦s actually a cool and useful piece of information. I am satisfied that you shared this helpful information with us. Please keep us up to date like this. Thanks for sharing.
Very nice post and right to the point. I don’t know if this is actually the best place to ask but do you folks have any ideea where to get some professional writers? Thank you 🙂
I loved as much as you will receive carried out right here. The sketch is tasteful, your authored material stylish. nonetheless, you command get bought an nervousness over that you wish be delivering the following. unwell unquestionably come further formerly again since exactly the same nearly a lot often inside case you shield this hike.
You are a very clever individual!
I as well believe thus, perfectly indited post! .
Your place is valueble for me. Thanks!…
What?s Happening i’m new to this, I stumbled upon this I’ve found It absolutely helpful and it has aided me out loads. I hope to contribute & aid other users like its aided me. Good job.
Thank you, I have recently been looking for information about this topic for ages and yours is the best I have discovered so far. But, what about the bottom line? Are you sure about the source?
It’s onerous to find educated folks on this topic, but you sound like you recognize what you’re talking about! Thanks
I?m not sure where you are getting your info, but great topic. I needs to spend some time learning more or understanding more. Thanks for great info I was looking for this info for my mission.
Heya just wanted to give you a quick heads up and let you know a few of the pictures aren’t loading properly. I’m not sure why but I think its a linking issue. I’ve tried it in two different internet browsers and both show the same outcome.
It?s in reality a nice and helpful piece of information. I?m glad that you shared this helpful information with us. Please keep us informed like this. Thank you for sharing.